Kurap atau ringworm adalah satu daripada penyakit kulit yang menjijikkan dan selalu dipandang hina dalam masyarakat Melayu. Sebab itu ada perumpamaan “seperti anjing kurap” dsb. Kurap mudah berjangkit dalam keadaan lembab terutamanya bagi kita yang duduk di kawasan tropika. Selain itu, berkongsi pakaian dengan orang yang berpenyakit ini juga menyebabkan kurap merebak dengan cepatnya. Yang jelasnya, kebersihan diri dan pakaian perlu dijaga untuk mengelakkan diri daripada dihinggapi oleh fungus penyebab kurap ini.
Oleh itu untuk mengetahui lebih lanjut mengenai kurap dan cara-cara untuk menghindarinya, di bawah ini dipanjangkan artikel berkaitan…
What is ringworm?
Ringworm is a common skin disorder otherwise known as tinea. While there are multiple forms of ringworm, the most common affect the skin on the body (tinea corporis), the scalp (tinea capitis), the feet (tinea pedis, or ‘athlete’s foot’), or the groin (tinea cruris, or ‘jock itch’).
Does ringworm mean I have worms?
Ringworm is not, as its name suggests, caused by a worm. Characterized by round lesions (rings) and early belief that the infection was caused by a parasite (worm), the term ringworm was born. Further confusion comes from the medical term for ringworm, tinea, which is Latin for ‘growing worm.’ While the condition is actually the result of a fungal infection, the name ‘ringworm’ has stuck.
What causes ringworm?
Although the world is full of yeasts, molds, and fungi, only a few cause skin problems. Ringworm fungi are known as dermatophytes — microscopic organisms that live off the dead tissues of your skin, hair, and nails, much like a mushroom can grow on the bark of a tree.
What types of ringworm are there?
As mentioned previously, there are several types of ringworm (tinea) that can affect different parts of the body. On the next several slides, we’ll take a look at the various forms from head to toe.
Ringworm of the body (tinea corporis)
When fungus affects the skin of the body, it often produces the round spots of classic ringworm. Sometimes, these spots have an “active” outer border as they slowly grow and advance. It is important to distinguish this rash from other even more common rashes, such as nummular eczema. This condition, and others, may appear similar to ringworm, but they are not fungal and require different treatment.
Ringworm of the scalp (tinea capitis)
Ringworm of the scalp commonly affects children, mostly in late childhood or adolescence. This condition may spread in schools. Tinea capitis appears as scalp scaling that is associated with bald spots (in contrast to seborrhea or dandruff, for instance, which do not cause hair loss).
Ringworm of the foot (tinea pedis)
Tinea pedis is an extremely common skin disorder. It is the most common and perhaps the most persistent of the fungal (tinea) infections. Also known as athlete’s foot, it may cause scaling and inflammation in the toe webs, especially the one between the fourth and fifth toes. Another common form of tinea pedis produces a thickening or scaling of the skin on the heels and soles as well as blisters between the toes or on the sole.
Ringworm of the groin (tinea cruris)
Tinea of the groin (‘jock itch’) tends to have a reddish-brown color and to extend from the folds of the groin down onto one or both thighs. Other conditions that can mimic tinea cruris include yeast infections, psoriasis, and intertrigo, a chafing rash which results from skin rubbing against skin.
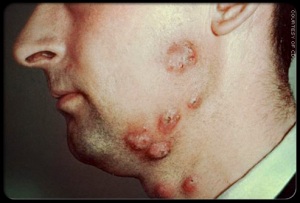
Ringworm of the beard (tinea barbae)
Ringworm of the bearded area of the face and neck, with swellings and marked crusting, often with itching, sometimes causes the hair to break off. In the days when men went to the barber daily for a shave, tinea barbae was called barber’s itch.
Ringworm of the face (tinea faciei)
Ringworm on the face outside of the beard area is called tinea faciei. On the face, ringworm is rarely ring-shaped. Characteristically, it causes red, scaly patches with indistinct edges.
Ringworm of the hand (tinea manus)
Ringworm may involve the hands, particularly the palms and the spaces between the fingers. It typically causes thickening (hyperkeratosis) of these areas, often on only one hand. Tinea manus is a common companion of tinea pedis (ringworm of the feet). It is also called tinea manuum.
Ringworm of the nails (tinea unguium)
This is the most common fungal infection of the nails, also called onychomycosis. It can make fingernails look white, thick, opaque, and brittle, but more often toenails look yellow, thick, and brittle. Artificial nails increase the risk for tinea unguium as emery boards can carry infection, and water can collect under the artificial nail, creating a moist, warm environment favorable for fungal growth.
How did I get ringworm?
Ringworm is highly contagious and can be spread multiple ways. You can get it from an infected person, animal, object, and even soil. Heat and moisture help fungi grow and thrive, which makes them more common in areas of frequent sweating as well as skin folds such as those in the groin or between the toes. This also accounts for their reputation as being caught from contaminated items such as toilet articles, clothing, pool surfaces, showers, and locker rooms.
Catching ringworm from pets.
Ringworm is an example of a zoonotic disease (transmitted from animals to humans). Cats are among the most commonly affected animals and studies have shown that in 30%-70% of households in which a cat develops ringworm, at least one person will develop the condition. Dogs, cows, goats, pigs, and horses can spread ringworm to humans and other animals via direct contact or contact with objects the infected animal has touched (such as bedding, grooming articles, saddles, furniture, carpeting, etc.).
How is ringworm diagnosed?
Sometimes, the diagnosis of ringworm is obvious from its location and appearance. Otherwise, skin scrapings for microscopic examination and a culture of the affected skin can establish the diagnosis of tinea or rule it out.
How is ringworm treated?
Ringworm can be treated topically with antifungal creams containing clotrimazole (Cruex, Desenex, Lotrimin), miconazole (Monistat-Derm), ketoconazole (Nizoral) and terbinafine (Lamisil). In severe or resistant infections on the scalp or nails, oral medications such as terbinafine, itraconazole (Sporanox), and fluconazole (Diflucan) are necessary.
Can ringworm be prevented?
Ringworm is difficult to prevent, but you can help reduce your risk by following some simple guidelines. The next several slides provide some helpful prevention tips in minimizing the chance of developing ringworm.
Ringworm Prevention Tip #1
Don’t share clothing, sports gear, towels, or sheets.
Ringworm Prevention Tip #2
Wear slippers or sandals in locker rooms and public pool & bathing areas.
Ringworm Prevention Tip #3
Shower and shampoo well after any sport that includes skin-to-skin contact.
Ringworm Prevention Tip #4
Wear loose-fitting cotton clothing. Change your socks and underwear at least once a day.
Ringworm Prevention Tip #5
Keep your skin clean and dry. Always dry yourself completely after showers or baths.
Ringworm Prevention Tip #6
If you have athlete’s foot, put your socks on before your underwear so that fungi do not spread from your feet to your groin.
Filed under: Kesihatan | 221 Comments »